Beware of Acute Flaccid Myelitis Between August-November

The US Centers for Disease Control and Prevention (CDC) anticipates that 2020 will be another peak year for cases of acute flaccid myelitis (AFM), a serious neurologic condition that affects mostly children.
Enteroviruses, particularly enterovirus-D68 (EV-D68), are likely responsible for these cases.
This uncommon disease has peaked every 2-years between August and November in the United States since 2014, stated the CDC on August 4, 2020.
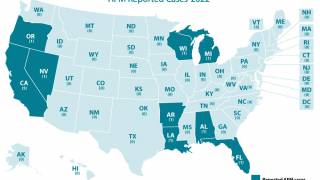
The 3rd and largest peak of AFM occurred in 2018, with 238 cases in 42 US states.
Thomas Clark, M.D., Deputy Director of CDC’s Division of Viral Diseases, said in a related press statement: “All clinicians should remain vigilant for AFM and promptly evaluate patients. During the COVID-19 pandemic, this may require adjusting practices to perform clinical evaluations of patients by phone or telemedicine.”
“However, clinicians should not delay hospitalizing patients when they suspect AFM.”
Pediatricians and frontline providers in emergency departments should be prepared to quickly recognize symptoms of AFM and immediately hospitalize patients. Timing is critical at each step—prompt AFM recognition leads to optimal medical management and early specimen collection.
AFM can progress rapidly over the course of hours or days, leading to permanent paralysis and/or the life-threatening complication of respiratory failure in previously healthy patients, so delays in care can be serious.
The CDC recently released a new Vital Signs report to alert healthcare providers to a possible outbreak this year. This Vital Signs report reveals a delay in care for some patients in 2018: 35% of patients were not hospitalized until 2+ days after limb weakness.
This Vital Signs report provides a more detailed view of clinical characteristics of AFM, which can help clinicians better recognize signs and symptoms, evaluate patients, and provide optimal medical management and rehabilitation.
Parents and doctors should suspect AFM in patients with sudden limb weakness, especially during August through November. Recent respiratory illness or fever and the presence of neck or back pain or any neurologic symptom should heighten their concern.
Laboratory tests and an MRI of the brain and spinal cord can distinguish AFM from other conditions with limb weakness.
Robert Redfield, M.D., CDC Director, added: “As we head into these critical next months, CDC is taking necessary steps to help clinicians better recognize signs and symptoms of AFM in children.”
The CDC’s latest review showed that in 2018:
- 76% sought medical care within one day, 64% presented to the emergency department
- 98% of patients with AFM were hospitalized
- 54% of patients were admitted to an intensive care unit; 1 in 4 hospitalized patients needed mechanical ventilation to help them breathe
- Most cases were in children (94%) and most patients (86%) had AFM onset during August through November. Most patients had a fever and/or respiratory illness approximately six days before limb weakness onset.
- Other common early symptoms were difficulty walking, neck or back pain, fever, and limb pain.
- While most patients were hospitalized within one day of limb weakness onset, 25% were not hospitalized until two to three days after, and 10% were not hospitalized until four or more days after their limb weakness began.
Enteroviruses, particularly enterovirus-D68 (EV-D68), is the most common virus identified among specimens collected from patients with AFM. However, other viruses can cause AFM and may also be contributing to the biennial peaks. Although AFM symptoms resemble those of polio, all specimens have tested negative for poliovirus.
There is currently no specific test, proven treatment, or prevention method for AFM.
To read more about the Nationwide Outbreak of Acute Flaccid Myelitis, the entire Vital Signs report is available.
Visit AFM for more information.
AMF news is reported by Precision Vaccinations.
Our Trust Standards: Medical Advisory Committee