Hepatitis C Screening For All Adults Now Recommended
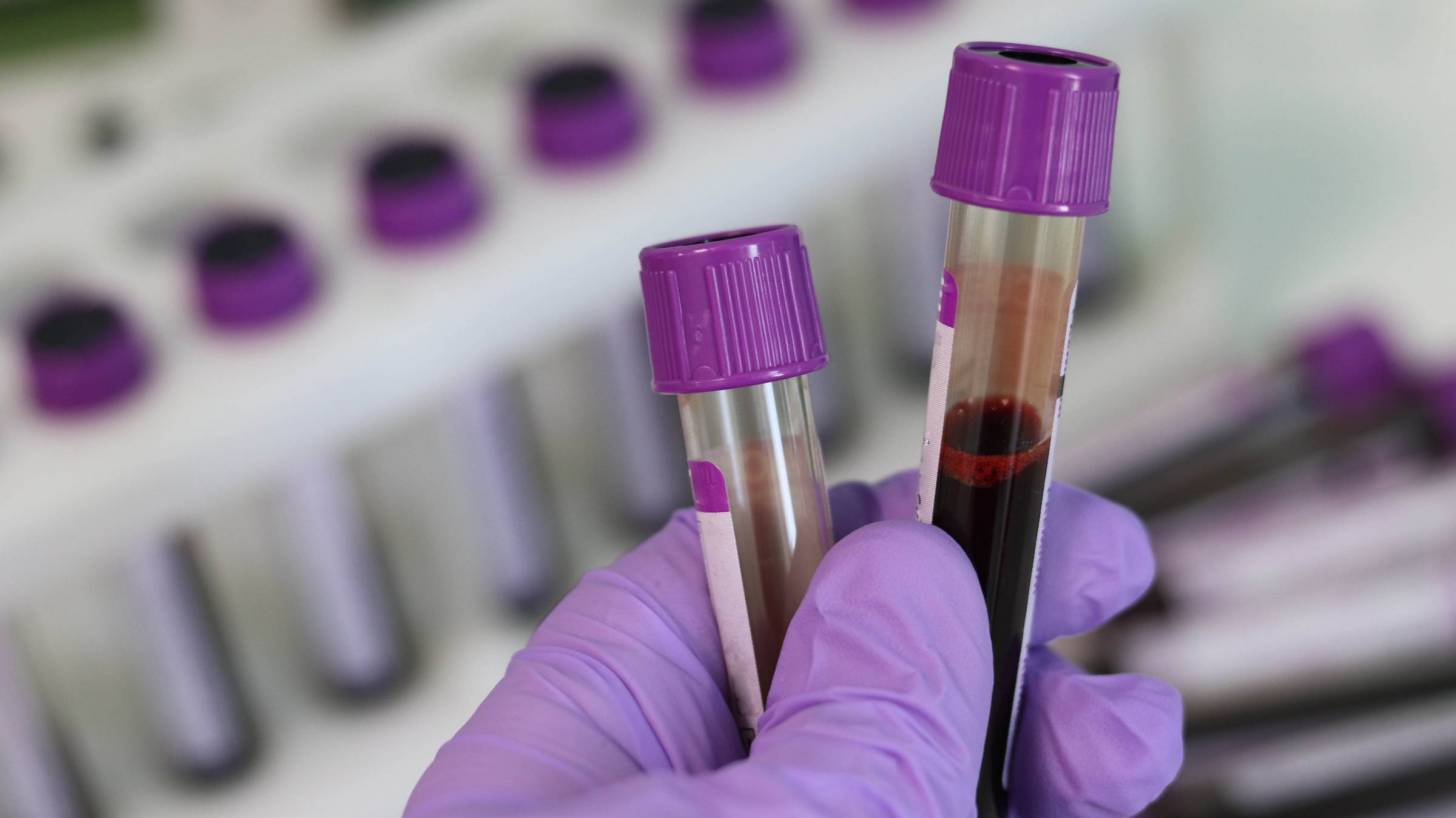
The U.S. Preventive Services Task Force (USPSTF) announced a draft recommendation for screening ‘all adults’ for the hepatitis C virus.
This announcement on August 27, 2019, says the Task Force concluded with "moderate certainty", a B recommendation, that there was a substantial net benefit in screening adults ages 18-79 for hepatitis C virus (HCV) infection.
The USPSTF cited ‘better treatments with direct-acting antiviral (DAA) therapy and increasing prevalence of HCV infection among younger adults’ as the reasons for this change of policy from 2013.
As of August 2019, there is no preventive vaccine available for the hepatitis C virus.
However, there is active research into the development of a vaccine for HCV.
Preventive vaccines are available for both hepatitis A and hepatitis B.
Furthermore, the USPSTF bases its recommendations on the evidence of both the benefits and harms of the service and an assessment of the balance.
However, the USPSTF does not consider the costs of providing a service in this assessment.
And, the USPSTF recognizes that clinical decisions involve more considerations than evidence alone. Clinicians should understand the evidence but individualize decision making to the specific patient or situation.
Similarly, the USPSTF notes that policy and coverage decisions involve considerations in addition to the evidence of clinical benefits and harms.
This is an important change since HCV is the most common chronic bloodborne pathogen in the United States and a leading cause of complications from chronic liver disease.
HCV infection is associated with more deaths than the top 60 other reportable infectious diseases combined, including HIV.
The public has an opportunity to offer comments on this page until September 23, 2019, at 8:00 PM EST.
The specifics of this recommendation are as follows:
Patient Population Under Consideration
- This recommendation applies to all asymptomatic adults without known liver disease.
Assessment of Risk
- Although all adults ages 18 to 79 years should be screened, a number of risk factors increase risk. The most important risk factor for HCV infection is past or current injection drug use. In the United States, recent increases in HCV incidence have predominantly been among young persons who inject drugs (PWID).
- Approximately one-third of PWID ages 18 to 30 years are infected with HCV, and 70% to 90% of older PWID are infected.
- Clinicians may want to consider screening in adolescents younger than age 18 years and in adults older than age 79 years who are at high risk.
- Pregnant adults should be screened.
- HCV prevalence has doubled in women ages 15 to 44 years from 2006 to 2014. From 2011 to 2014, 0.73% of pregnant women tested had an HCV infection, with a 68% increase in the proportion of infants born to HCV-infected mothers.
- Approximately 1,700 infected infants are born annually to 29,000 HCV-infected mothers.
- Due to the increasing prevalence of HCV in women ages 15 to 44 years and in infants born to HCV-infected mothers, clinicians may want to consider screening pregnant persons younger than age 18 years.
Screening Tests
- Screening with anti-HCV antibody testing followed by polymerase chain reaction testing for HCV RNA is accurate for identifying patients with chronic HCV infection. Currently, diagnostic evaluations are often performed with various noninvasive tests as possible alternatives to liver biopsy for diagnosing fibrosis stage or cirrhosis to reduce overall harms in persons who screen positive.
- Among patients with abnormal results on liver function tests (measurement of aspartate aminotransferase, alanine aminotransferase, or bilirubin) who were tested for reasons other than HCV screening, finding the cause of the abnormality often includes testing for HCV infection, and is considered case finding rather than screening; therefore, it is outside the scope of this recommendation.
Screening Intervals
- Most adults need only be screened once. Persons with continued risk for HCV infection (e.g., PWID) should be screened periodically.
- There is limited information about the specific screening interval that should occur in persons who continue to be at risk for new HCV infection.
Screening Implementation
- The USPSTF believes that screening should be voluntary and undertaken only with the patient's knowledge and understanding that HCV screening is planned.
Treatment
- The purpose of antiviral treatment regimens for HCV infection is to prevent long-term health complications of chronic HCV infection (such as cirrhosis, liver failure, and hepatocellular carcinoma).
- Currently, oral direct-acting antiviral (DAA) regimens without interferon have been accepted as the standard treatment of chronic HCV infection.
- Antiviral therapy is not generally considered during pregnancy because of the lack of data on the safety of newer DAA regimens during pregnancy and breastfeeding.
The most important risk factor for HCV infection is past or current injection drug use.
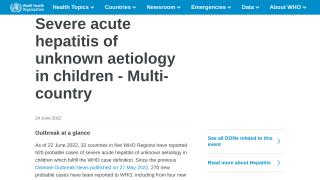
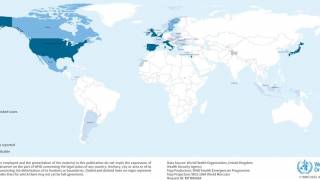
In the United States, an estimated 4.1 million persons have past or current HCV infection. Of these persons with antibodies, approximately 2.4 million have current infections based on testing with molecular assays for HCV RNA.
"While research into a new vaccine offers hope, current treatment options for hepatitis C have a much higher success rate than therapy options in the past, but we cannot treat patients that we don’t know about," said Chris Felton, PharmD, Clinical Pharmacist, MTM and Immunization Specialist for Brookshire's Grocery Company.
"Patients need to be identified, and clear screening guidelines are essential."
>> Private Hep C Test Services <<
An estimated 41,200 new HCV infections occurred in the United States in 2016.
Cases of acute HCV infection have increased approximately 3.5-fold over the last decade.
The increase in acute HCV incidence has mostly affected young, white persons who inject drugs, especially those living in rural areas.
Additionally, there has also been an increase in the number of women ages 15 to 44 years with HCV infection, said the USPSTF.
Published by Precision Vaccination
Our Trust Standards: Medical Advisory Committee