HepC Services and State Laws Often Don’t Match

Various changes over the past decade have reshaped the Hepatitis C virus epidemic in the USA.
This is important news since Hepatitis C virus infections are the most frequently reported blood-borne infection in the USA.
And, approximately 18,000 people died in 2016 because of Hepatitis C infection, says the Centers for Disease Control and Prevention (CDC).
With the increasing availability of direct-acting antivirals, public health strategies have raised the elimination of Hepatitis C as a possible goal.
However, there is not a Hepatitis C vaccine available to help reach this goal.
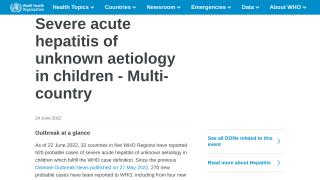
To better understand the geographic differences of Hepatitis C virus (HCV) in certain sections of the USA, a new study estimated that the national prevalence from 2013 to 2016 was 0.93 percent among adults in the noninstitutionalized US population, which corresponds to approximately 2,260,000 persons with a current infection.
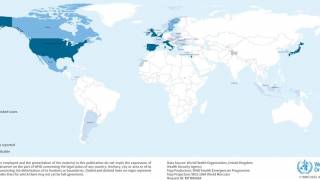
Nine states contained 51.9 percent of all persons living with HCV infection, led by California (318,900), Texas (202,500), Florida (151,000), and New York (116,000).
But, 3 of the top 10 states with the highest HCV prevalence were located in ‘Appalachia’.
The states of Kentucky, Tennessee, and West Virginia together constituted 5.8 percent of persons with HCV, but just 4.0 percent of the USA population.
In Appalachia, it is likely that HCV prevalence reflects recent increases in injection drug use, high densities of counties vulnerable to HCV and HIV infection outbreaks, large outbreaks of these infections among persons who inject drugs (PWID), and elevated reports of acute HCV.
According to these researchers, these findings were consistent across analyses that considered alternative incidence rates for the highest-prevalence 1945 to 1969 cohort and alternative approaches for populations not included in the NHANES sampling frame.
These estimates help to quantify the need for investments in services for the prevention of HCV.
This includes syringe services programs, which are associated with decreased HCV spread, especially when combined with linkage to medication-assisted substance use treatment.
Although increasing, the number of syringe services programs remains low in 2018 in many states, with programs often geographically dispersed within states.
Direct medical services such as HCV testing and curative treatments remain cornerstones for extending life and averting transmission, said this research.
Furthermore, testing and treatment are cost-effective, with earlier treatment possibly yielding greater cost savings, reported these researchers.
But, some state policies restrict the availability of these services.
A separate analysis found substantial variation in the laws supporting access to clean injection equipment and People who inject drugs, of Medicaid fee-for-service HCV treatment.
In summary, this research found some of the highest-incidence states for HCV had the lowest levels of prevention and treatment access.
Overall, this study reported 47 states were found lacking comprehensive laws and Medicaid policies for effective prevention and treatment of HCV among PWID(People who inject drugs).
This study was supported by the CDC National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention Epidemic and Economic Modeling Agreement (grant U38 PS004646) (Dr. Rosenberg, Ms. Rosenthal, and Mr. Hall) and the Center for AIDS Research at Emory University (grant P30AI050409).
These researchers disclosed various relationships.
Corresponding Author: Eli S. Rosenberg, Ph.D., Department of Epidemiology and Biostatistics, University at Albany School of Public Health, State University of New York, Rensselaer, NY 12144 ([email protected]).
Our Trust Standards: Medical Advisory Committee
- Population-level Outcomes and Cost-Effectiveness of Expanding the Recommendation for Age-based Hepatitis C Testing in the US
- State HCV Incidence and Policies Related to HCV Preventive and Treatment Services for Persons Who Inject Drugs — United States
- Prevalence of Hepatitis C Virus Infection in US States and the District of Columbia, 2013 to 2016
- Do direct acting antivirals cure chronic hepatitis C?
- Hepatitis C