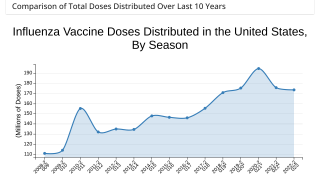
Does Influenza Virus Imprinting Influence Severe Hospitalizations

A recent study revealed that despite more influenza A(H3N2) related hospitalizations, patients hospitalized with flu A(H1N1)pdm09 or B viruses had a higher likelihood of in-hospital severe outcomes.
Before this U.S. Centers for Disease Control and Prevention (CDC) funded study was published, little was known about the relative severity of flu infections by influenza virus type and subtype in hospitalized people.
Published in The Lancet Microbe on September 25, 2023, this study found that about 17% of people hospitalized with influenza had severe outcomes such as intensive care unit (ICU) admission, use of invasive mechanical ventilation, or extracorporeal membrane oxygenation (MV/ECMO) over nine flu seasons.
Compared to hospitalizations with flu A(H3N2) virus, people hospitalized with flu A(H1N1)pdm09 virus were:
- 42% more likely to be admitted to the ICU
- 79% more likely to receive MV/ECMO
- 25% more likely to die
Compared to hospitalizations with flu A(H3N2) virus, people hospitalized with flu B virus were:
- 6% more likely to be admitted to the ICU
- 14% more likely to receive MV/ECMO
- 18% more likely to die
Similar increases in the likelihood of ICU admission and MV/ECMO use were seen for people of all ages hospitalized with A(H1N1)pdm09 viruses. However, results were variable by age for influenza B.
These researchers looked at flu-related hospitalizations from the 2010─2011 through 2018─2019 flu seasons from FluSurv-NET sites in 13 states. The FluSurv-NET system represents over 29 million people or approximately 9% of the U.S. population.
Of the 104,969 flu-related hospitalizations captured by the FluSurv-NET system:
- 52% of people were vaccinated against flu.
- 88% of people had at least one comorbid condition.
- ICU admission occurred in 16.7%, MV/ECMO use in 6.5%, and death in 3%.
These researchers wrote that differences in the association between virus type or subtype and death across age groups could be partly explained by immune imprinting of the specific influenza viruses that individuals were first exposed to in childhood.
A previous study published in 2019 concluded newer and less "senior" antibody responses acquired later in life do not provide the same strength of protection as responses imprinted in childhood.
However, an evaluation of the effect of immune imprinting on influenza severity was outside the scope of this study but could be investigated in future work.
Furthermore, no association between influenza type or subtype and odds of death was noted in vaccinated individuals, highlighting the importance of receiving the annual influenza vaccine to protect against severe illness.
Vaccine effectiveness is typically lower for influenza A H3N2 than for A H1N1pdm09 virus, which, when not accounted for, would increase the likelihood of individuals having more severe A H3N2 virus infections.
This study's findings highlight the importance of the CDC's recommendation that most people get an annual flu shot and early antiviral treatment for patients at increased risk of severe flu, no matter which flu viruses are circulating.
Our Trust Standards: Medical Advisory Committee
- Severity of influenza-associated hospitalisations by influenza virus type and subtype in the USA, 2010–19:
- Childhood immune imprinting to influenza A shapes birth year-specific risk during seasonal H1N1 and H3N2 epidemics
- Influenza Virus H1N1pdm09 Infections in the Young and Old: Evidence of Greater Antibody Diversity and Affinity for the Hemagglut
- CDC Study Looks at Flu Severity by Virus Type and Subtype