Oral Related Cancer Cases Increase

During 2007–2016, the incidence of cancers of the oral cavity and pharynx increased, despite decreases in several anatomic sites, including the nasopharynx, hypopharynx, lip, and the floor of the mouth.
According to this study published by the Centers for Disease Control and Prevention (CDC) on April 17, 2020, the overall increase appears to be driven by increases in cancers of the tonsil, base of tongue, oropharynx, and other cancers of the oral cavity and pharynx.
These cancers are associated with Human Papillomavirus (HPV), as well as by those of gum and anterior tongue.
By age group, rates for all cancers of the oral cavity and pharynx combined increased among persons aged 50–79 years, decreased among those aged 40–49 years, and were stable among those aged between 20–39 and over 80 years of age.
The continued declines in tobacco use might have contributed to the decreases observed in some sites.
Population-based tobacco control measures are proven to prevent tobacco use initiation and promote smoking cessation, but they are not implemented equally in all U.S. states and communities.
To reduce the risk for cancers of the oral cavity and pharynx, which account for about 3 percent of cancers diagnosed annually in the USA, communities might benefit from a broader application of evidence-based interventions and targeted efforts among groups with a high prevalence of tobacco and alcohol use or high cancer rates.
A previous study found rates of oropharyngeal squamous cell cancers increased the most among white men compared with other racial/ethnic groups.
Differences in sexual behavior might account for the higher rate; compared with other racial/ethnic groups.
White men report an earlier age at oral sex initiation and have a higher number of oral sex partners, which have been shown to be risk factors for exposure to HPV infection.
HPV is the most common sexually transmitted infection in the USA, and persistent infection with certain types of the virus can cause cancer. About 14 million people, including teens, become infected with HPV each year.
Furthermore, public health efforts that focus on increasing HPV vaccination are an essential component of cancer prevention.
Routine HPV vaccination is recommended for all persons at age 11 or 12 years, with catch-up vaccination through age 26 years.
Recently, a study published by researchers at The University of Texas Medical Branch at Galveston indicates that just 1-dose of a HPV vaccine is as effective as multiple vaccinations for preventing pre-invasive cervical disease.
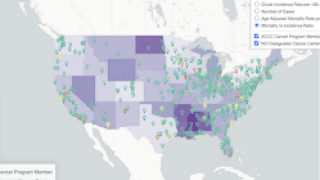
The CDC’s National Comprehensive Cancer Control Program supports cancer prevention efforts in all 50 states, the District of Columbia, tribal organizations, and U.S. territories; and, in collaboration with CDC’s National Center for Immunization and Respiratory Diseases, support activities to promote and provide access to HPV vaccine.
Note: There are no data on the efficacy of HPV vaccination on oral cavity and pharyngeal cancers from clinical trials. However, these cancers are caused by HPV types that are targeted by available vaccines.
The findings in this report are subject to at least three limitations.
- First, delays in cancer reporting might result in an underestimate of incidence.
- Second, cancer registries do not routinely collect or report information about risk factors such as HPV infection, tobacco use, or alcohol use, so it was not possible to determine whether cancers occurred in persons exposed to these risk factors.
- Finally, because of the complexity of this anatomic region and potential difficulty in determining precisely where cancer originated, the anatomic site for some cases might have been incorrectly classified.
All vaccines used in the USA, including HPV vaccines, are required to go through years of extensive safety testing before they are licensed by the U.S. Food and Drug Administration.
The Gardasil 9 vaccine consists of HPV proteins, Types 6, 11, 16, 18, 31, 33, 45, 52, and 58, amorphous aluminum hydroxyphosphate sulfate, yeast protein, sodium chloride, L-histidine, Polysorbate 80, sodium borate, and water for injection.
These researchers did not disclose any industry conflicts of interest.
HPV vaccine news published by Precision Vaccinations.
Our Trust Standards: Medical Advisory Committee