Bisexual and Gay Men Benefit from HPV Vaccination

A new study led by Monash University and Alfred Health found a 70% reduction in one type of human papillomavirus (HPV) in gay and bisexual men after the implementation of an HPV vaccination program in 2013.
Published in Lancet Infectious Diseases on May 24, 2021, the HYPER2 study found a significant reduction in vaccine-preventable HPV genotypes in men who have sex with men (MSM) aged 16-20 years following the introduction of the vaccine.
And the decrease in anal HPV 16 and 18 may lead to a reduction in the incidence of anal cancer.
This study included 400 MSM with a median age of 19 years from sexual health clinics, and the community in Melbourne, with a median number of lifetime male partners, was ten.
The prevalence of any anal quadrivalent vaccine-preventable HPV genotype was higher in the pre-vaccination cohort (54 [28%] of 193) than in the post-vaccination cohort (14 [7%] of 193; adjusted prevalence ratio [PR] 0·24, 95% CI 0·14–0·42), primarily driven by decreases in HPV6, followed by HPV 11, 16, and 18.
Nevertheless, there was also a significant reduction in anal HPV16 and 18 in the post-vaccination cohort from the pre-vaccination cohort (0·31, 0·14–0·68).
The prevalence of any penile quadrivalent vaccine-preventable HPV genotype was also higher in the pre-vaccination cohort (21 [12%] of 177) than in the post-vaccination cohort (11 [6%] of 179; 0·48, 0·24–0·97), driven by decreases in HPV 6 and 11, but not by 16 and 18.
The prevalence of any oral quadrivalent vaccine-preventable HPV genotype was higher in the pre-vaccination cohort than in the post-vaccination cohort, and there were no cases of oral HPV 6 or 11 detected in the HYPER2 study.
When comparing the pre-vaccinated cohort with the 149 confirmed vaccinated men from HYPER2 showed a reduction in any quadrivalent vaccine-preventable HPV genotype for anal (0·09, 0·03–0·25) and penile (0·18, 0·05–0·59) infection, but not for oral infection (0·17, 0·03–1·08).
Australia is one of the first countries that offered both boys and girls vaccination programs for HPV.
The HPV vaccine used in this program covers four genotypes: 6/11/16/18. Genotypes 6/11 cause about 90% of the genital wart cases, and genotypes 16/18 cause about 70% of cervical and anal cancers.
“Australia has a very successful HPV vaccination program for both boys and girls with high vaccine coverage,” Associate Professor Eric Chow stated in a press release.
“The vaccine is effective in reducing HPV-related diseases and showing some promising evidence that this may lead to a reduction in HPV-related cancer in the future.”
This study was funded by Merck, which produces HPV vaccines, and the Australian Government Department of Health.
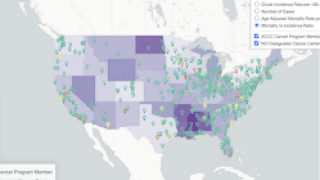
In the USA, nearly 35,000 people are estimated to be affected by cancer caused by HPV infection each year. While there is screening for cervical cancer that can detect cancer early, there is no recommended screening for the other cancers caused by HPV infection, like cancers of the back of the throat, anus, penis, vagina, or vulva.
There are safe and effective HPV vaccines to protect males and females against cancers caused by HPV. These vaccines include 9vHPV, 4vHPV, and/or 2vHPV, says the US Centers for Disease Control and Prevention (CDC).
In the USA, HPV vaccination for adolescents has been recommended for females since 2006 and for males since 2011, says the CDC.
CDC recommends HPV vaccination for children ages 11 or 12 years to protect against cancers caused by HPV infections. Vaccination can be started at age nine and is recommended through age 26 years for those not adequately vaccinated previously.
PrecisionVaccinations publishes research-based HPV vaccine news.
Our Trust Standards: Medical Advisory Committee