TB Vaccine Found 2X Effective as Previously Reported
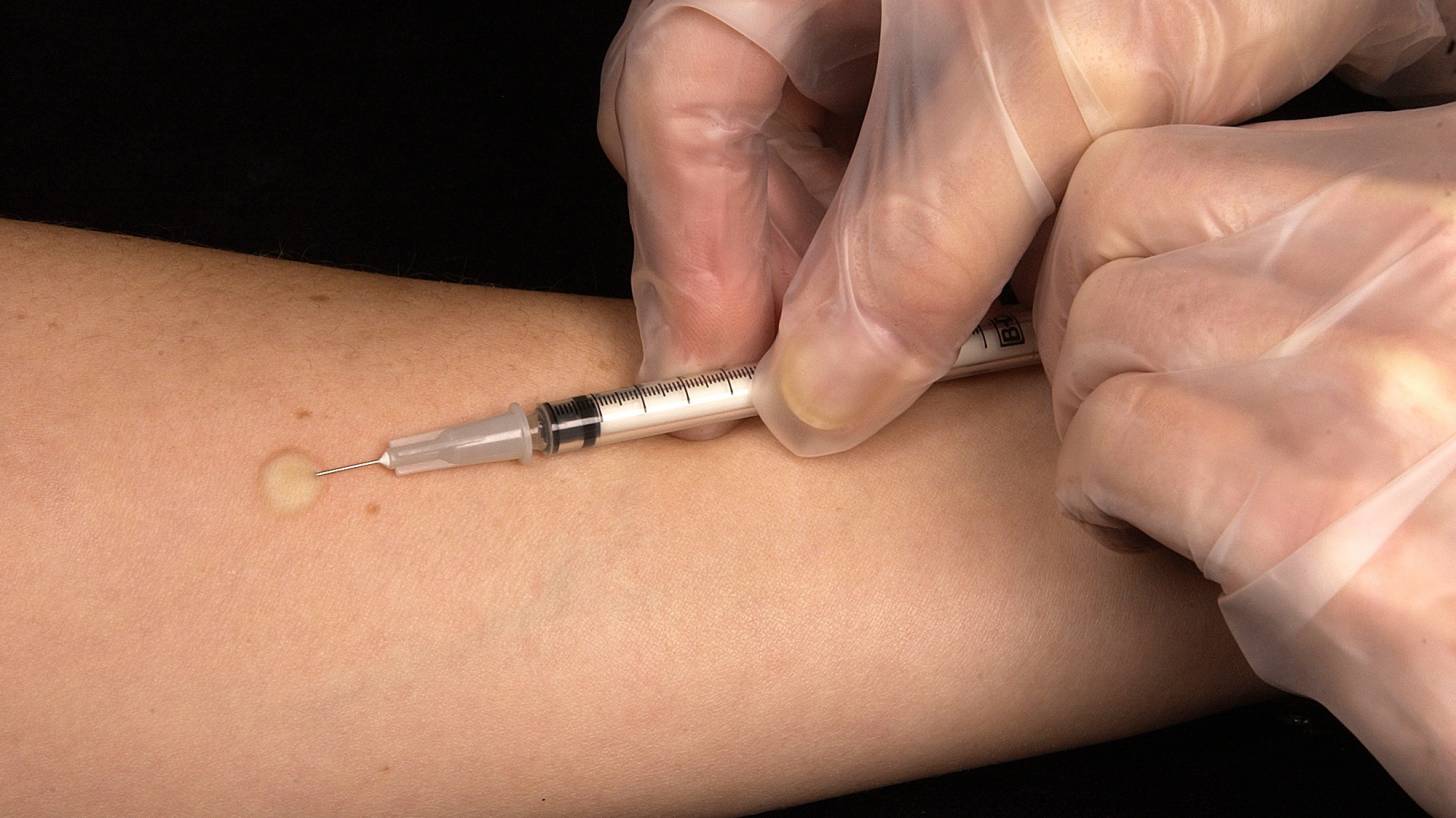
A 96-year-old vaccine has reaffirmed it is still the best prevention. The only vaccine against tuberculosis has been found to be more effective than previously reported.
Named after the French scientists who developed it, Bacillus Calmette-Guérin (BCG) was first used in 1921, and had been classified to work for only 10 to 15 years.
But researchers say they have found that the BCG vaccine protects half of those who received the vaccination by the age of 12 were still protected for at least 20 years.
Lead author Dr. Punam Mangtani, Associate Professor in Epidemiology at the London School of Hygiene & Tropical Medicine, said: "Tuberculosis kills nearly two million people every year, more than HIV/AIDS, but TB prevention methods have changed little in half a century."
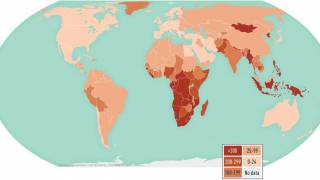
With no alternative vaccine for TB imminently available, these researchers say their findings provide an argument for uptake to be higher in areas where TB risk is high but vaccination coverage is low, such as parts of Central and Western Africa, East Asia and the Pacific.
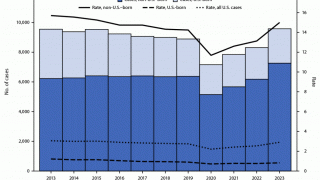
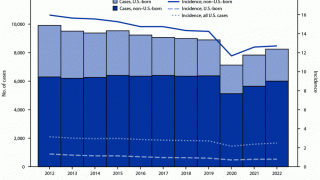
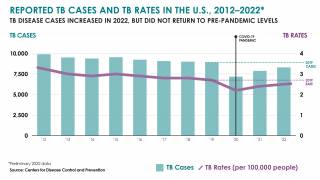
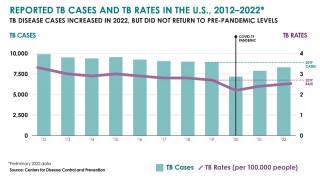
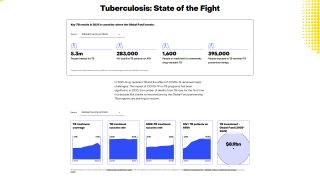
In 2015 there were an estimated 10.4 million new cases of TB and 1.8 million deaths globally.
Tuberculosis is caused by a bacterium called Mycobacterium tuberculosis. The bacteria usually attack the lungs, but TB bacteria can attack any part of the body such as the kidney, spine, and brain. Not everyone infected with TB bacteria becomes sick.
As a result, two TB-related conditions exist: latent TB infection (LTBI) and TB disease. If not treated properly, TB disease can be fatal.
Two to three billion of the world's population are infected with Mycobacterium tuberculosis, 10% of whom progress to clinical disease.
In the UK, BCG vaccination was given mostly to schoolchildren until it was discontinued in 2005 as the risk of TB was low. It has continued to be recommended for babies and infants who are at higher risk.
BCG vaccine is given in infancy with an estimated 88% coverage overall.
Its protective effect can be lower closer to the equator where environmental non-tuberculous mycobacteria or TB infection are more common and, if the infection occurs before the vaccination, can mask or block its effect.
Although the World Health Organization's End TB strategy highlights the importance of continuing infant BCG vaccination in high prevalence settings, this study suggests it may have a bigger role to play.
Dr Mangtani said: "Health officials should consider recommending childhood BCG vaccination where TB risk is high and where infant vaccination has not been given.”
“BCG is not perfect but until a new, more effective vaccine is approved and rolled-out, we should be maximising its potential. We should also be supporting the various agencies that make sure BCG is readily available globally."
The authors acknowledge limitations of the study, including not being able to exclude subjects who had positive tuberculin skin test in the school vaccination programme who would have been ineligible for vaccination, and that subjects taking part are more likely to have been vaccinated than those not contactable or who had refused.
The research was led by the London School of Hygiene & Tropical Medicine and funded by the National Institutes of Health Research Health technology Assessment (NIHR HTA) grant no 08/17/01.
These researchers did not report any conflicts of interest: Punam Mangtani Patrick Nguipdop-Djomo Ruth H Keogh Jonathan AC Sterne Ibrahim Abubakar Peter G Smith Paul EM Fine Emilia Vynnycky John M Watson David Elliman Marc Lipman Laura C Rodrigues.
Our Trust Standards: Medical Advisory Committee