Low Vaccination Rates Fueled NYC’s Last Measles Outbreak

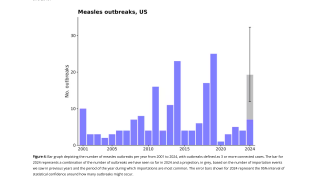
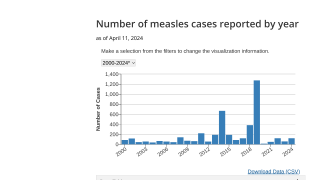
An analysis of the 2018-2019 measles outbreak in New York City (NYC), the largest such outbreak in the United States in nearly 30 years, identifies factors that made the outbreak so severe.
Furthermore, this new analysis published on May 27, 2020, highlights the prospective health risks to NYC’s children, as overall vaccination rates have diminished during the COVID-19 disease outbreak.
As of May 15, 2020, the Vaccine Tracking System indicates a notable decrease in orders for measles-containing vaccines.
This decline began the week after the COVID-19 national emergency was declared on March 13, 2020.
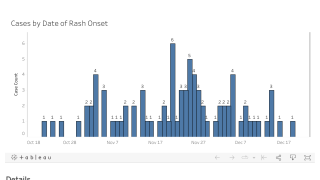
Using a model inference system, these researchers reconstructed in detail the transmission dynamics of the measles outbreak in an Orthodox Jewish community in NYC from October 2018 to July 2019.
Using model simulation and the posterior estimates from the model inference system, we are also able to estimate the impact of vaccination campaigns implemented during the outbreak, including numbers of infections and hospitalizations averted.
This analysis estimated that around a quarter of young children aged 1 to 4 in the affected community were susceptible at the onset of the outbreak, likely due to delayed vaccination.
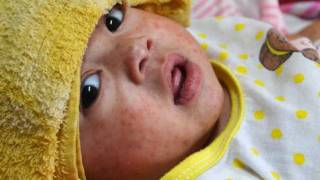
Specifically, 94 percent (101 of 108) of the early measles infections in children were those who were unvaccinated.
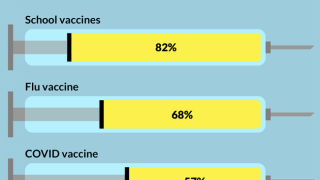
In contrast, the vaccination rate remained high in older children 5 to 17 years, with an estimated 94 percent immune to measles.
This difference may be due to better compliance with vaccination regulations, such as at school entry.
Nevertheless, this observation highlights the importance of vaccination compliance with both of the Measles-Mumps-Rubella (MMR) vaccine doses, especially given the long lag-time between the doses.
In addition, recommending the 2nd MMR vaccine dose earlier than the currently scheduled age 4 to 6 years could allow parents to fully vaccinate their children sooner and reduce the number of susceptible children overall.
This study also reveals the intricate interplay of population dynamics and measles transmission.
While the high susceptibility in children under 4 was likely responsible for the early spread of measles, the estimates suggest that the second and more severe part of the outbreak in 2019 was likely due to increased infectious contact (lack of social distancing) among this age group.
In addition, the intensified measles outbreak affected not only children with delayed vaccination but also a large number of infants under 1, who were too young to receive their 1st dose of MMR vaccine in the United States.
At least 100 infants under 1 were infected with measles during the 10-month outbreak period, despite extensive infection and transmission control efforts, including vaccinating infants 6 months or older and postexposure prophylaxis with immune globulin given to those under 6 months.
This was largely a result of the high susceptibility, and low natural immunities, in infants.
In addition, the simulations suggest that, without the vaccination campaigns, the number of infections in infants could have been over 10 times higher than observed.
These findings demonstrate the rippling effects of vaccine hesitancy beyond the risk posted to age-eligible children with delayed vaccination.
In summary, these researchers said ‘Our model simulations, consistent with many previous studies, demonstrate the significant public health impact of vaccination in controlling measles outbreaks.’
‘Without the implemented vaccination campaigns, the severity of the measles outbreak, including the number of infections, hospitalizations, and severe infections needing intensive care, could have been over 10x worse than observed.’
The study was funded by a grant from the National Institute of Allergy and Infectious Diseases (AI145883). No conflicts of interest were disclosed.
Measles vaccination news published by PrecisionVaccinations.
Our Trust Standards: Medical Advisory Committee