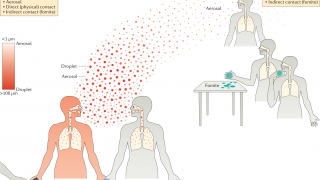
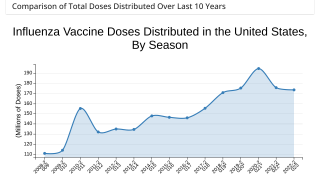
Why is FluMist Nasal Vaccine Available in Canada and the UK, But Not the USA?

Researchers have discovered a genetic mutation in the FluMist intranasal flu vaccine that has the potential to be altered, which would then enhance the vaccine’s protective effect.
Over the past 2 years, the Advisory Committee on Immunization Practice (ACIP) found that the FluMist vaccine had grown less effective in the USA, possibly due to shifts in circulating flu strains.
The ACIP’s recommendation led the Centers for Disease Control and Prevention (CDC) to say FluMist should not be used in the U.S. for the past 2 years.
FluMist Quadrivalent was originally approved in the US in 2003. According to the ACIP, the efficacy problem with FluMist began in 2013, specifically relating to one component of the influenza A virus, known as H1N1.
FluMist continues to be available in both Canada and the UK.
But, this new study may offer some hope for FluMist’s availability … maybe next year.
Researchers from the Bloomberg School discovered a previously overlooked mutation, present within two of the viral strains used in the vaccine, that reduces virus production.
“We had studied M2 for years, but one day recently a student in my lab noticed that the M2 in the LAIV influenza A viruses contain a mutation in the same part of the protein that we had previously identified as affecting viral replication,” says Andrew S. Pekosz, PhD, professor in the Bloomberg School’s Department of Molecular Microbiology and Immunology.
When the researchers reversed the mutation in one of the viruses, the virus became more active, making copies of itself, known as replicating, more quickly in cultured human nasal cells.
This change induced a stronger production of immune proteins.
“Only one component of FluMist – the one targeting the Type A H1N1 virus – has been failing in the U.S. recently,” said Dr. Pekosz.
“It’s not clear exactly why it has failed but this mutation we identified could be used to make that component of the vaccine a little stronger, thereby improving vaccine efficacy. We now see the possibility of altering this mutation and perhaps others in the vaccine to optimize the vaccine’s protective effect, perhaps for different age groups,” said Dr. Pekosz.
The FluMist vaccine, also known as LAIV (live, attenuated influenza vaccine) is made from four weakened flu virus strains, two representing the influenza A type, and two representing the influenza B type.
Two segments of the strains used in the vaccine are altered periodically to match the strains of influenza circulating in the population.
The non-varying parts of the vaccine are made from a special, cold-adapted H2N2 strain that is known to contain mutations that slow its replication at the temperatures found in the human nose and throat.
That slowing of activity is largely what keeps these vaccine strains from causing illness in people, although they remain active enough to induce at least partial immune protection against future influenza A infections.
Scientists in previous studies have linked the slower replication of this cold-adapted strain to changes in three virus genes.
“What we’re trying to do now is make a panel of these LAIV viruses with different mutations to see if we can boost the replication rates to get vaccine formulations that protect children and other age groups better than LAIV has done in the past few years,” Dr. Pekosz says.
“The M2 protein of live, attenuated influenza vaccine encodes a mutation that reduces replication in human nasal epithelial cells” was written by Nicholas Wohlgemuth, Yang Ye, Katherine J. Fenstermacher, Hsuan Liu, Andrew P. Lane, and Andrew Pekosz. These researchers did not disclose any conflicts of interest
The CDC recommends that everyone 6 months and older get an injectable flu vaccine as soon as possible.
Most pharmacies in the USA offer several FDA approved flu vaccines.
The flu shot cost varies depending on your insurance and which state you live.
The CDC Vaccine Price List provides the private sector vaccine prices for general information.
Flu vaccine discounts can be found here.
Support for the research was provided by the U.S. National Institutes of Health (R01 AI097417, HHSN272201400007C, R01 AI072502 and T32 AI007417) and the Shikani/El Hibri Prize for Discovery and Innovation.
Media contacts for the Johns Hopkins Bloomberg School of Public Health: Barbara Benham at 410-614-6029 or [email protected].
Our Trust Standards: Medical Advisory Committee