Diagnosing Latent Tuberculosis Infection
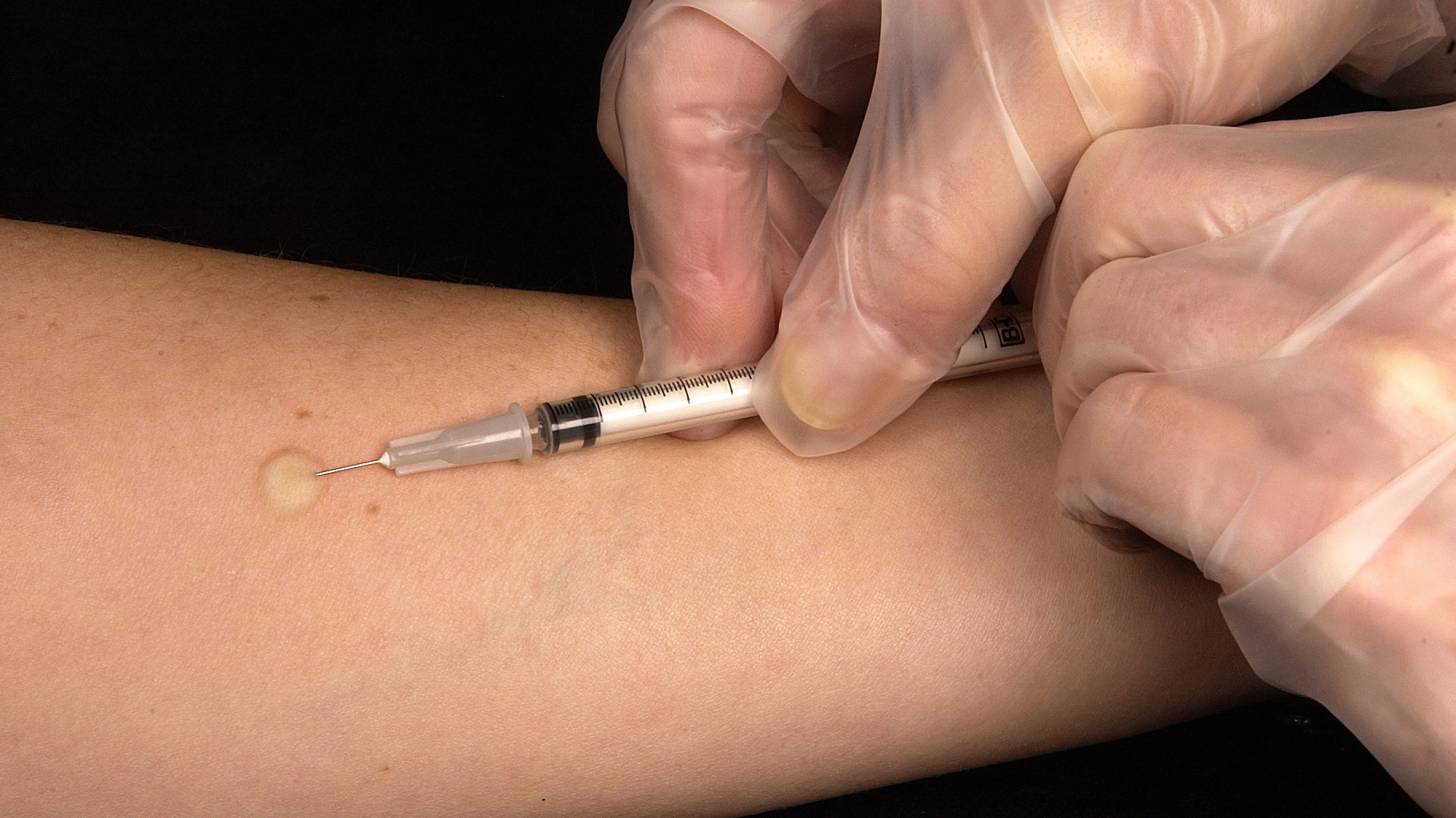
Most Mycobacterium tuberculosis infections in children and adolescents are asymptomatic, which is commonly known as latent.
After exposure to a person with active tuberculosis, some people will become infected and others will not.
Initially, the two groups cannot be distinguished, said H. Cody Meissner, M.D., FAAP, in an American Academy of Pediatrics news article, published November 27, 2018.
Ten weeks after exposure, people who become infected will demonstrate a positive tuberculin skin test (TST) or a positive interferon gamma release assay (IGRA).
Among exposed people who are not infected, the TST or IGRA will remain negative.
Tuberculosis infection, in contrast to tuberculosis disease, is defined as an infection in a person with a positive IGRA or TST but no physical findings of disease and a chest radiograph that is normal or reveals evidence of an old, healed infection.
The Food and Drug Administration has licensed two IGRAs to assist in diagnosing M. tuberculosis infections.
An IGRA measures interferon release from lymphocytes exposed to specific antigens found on M. tuberculosis. The antigens used in the IGRA do not cross-react with antigens in the BCG vaccine.
White blood cells (WBCs) from most people who have been infected with M. tuberculosis will release gamma interferon when mixed in vitro with antigens derived from M. tuberculosis.
The amount of gamma interferon released or the number of cells that release gamma interferon can be measured to determine the likelihood of infection.
WBCs from a person who has not been infected will not release gamma interferon when exposed to these antigens.
The sensitivity of IGRA and TST are similar, but the specificity of the IGRA generally is greater than that of the TST because the antigens used in the IGRA are not found in BCG or most nontuberculous mycobacteria.
Neither IGRA nor TST differentiates between latent tuberculosis infection and active disease.
Data suggest IGRA results are reliable in children 2 years of age or older.
If the IGRA result is negative but the TST result is positive in an asymptomatic, unexposed child, infection by M. tuberculosis is unlikely.
The advantages of an IGRA include the following:
- need for only one visit (useful for people from groups that historically have poor rates of return for TST reading) and,
- the fact that prior BCG vaccination does not cause a false-positive result.
The limitations of the assay include higher cost than TST, limited experience in children younger than 2 years and limited usefulness in immunocompromised children.
IGRAs can be used in place of the TST in all situations where testing for tuberculosis is recommended. Because of possible interference from live virus vaccines, TST or IGRA testing should be performed on the same day as live vaccine administration or four to six weeks later.
Lack of reaction to a TST or a negative IGRA result does not exclude infection by M. tuberculosis.
Young age, poor nutrition, immunosuppression, certain viral infections, disseminated tuberculosis and infection beginning less than three months previously may influence either test result.
For children younger than 2 years of age, the TST (Mantoux) generally is preferred for testing for the diagnosis of latent or active M. tuberculosis infection.
In a child 2 years or older who was BCG vaccinated and has a positive tuberculin skin test, an IGRA can help differentiate tuberculosis infection from positivity attributable to the Bacille Calmette-Guerin (BCG) vaccine.
BCG is a vaccine for tuberculosis disease.
Many foreign-born persons have been BCG-vaccinated. BCG is used in many countries with a high prevalence of TB to prevent childhood tuberculous meningitis and miliary disease, says the Centers for Disease Control and Prevention (CDC).
However, BCG is not generally recommended for use in the United States because of the low risk of infection with Mycobacterium tuberculosis, the variable effectiveness of the vaccine against adult pulmonary TB, and the vaccine’s potential interference with tuberculin skin test reactivity.
A positive IGRA result should be interpreted as evidence that a child has a tuberculosis infection.
However, a negative IGRA alone cannot be interpreted as a reason to exclude tuberculosis infection.
Indeterminate/invalid IGRA results should not be used to determine the need for anti-tuberculosis therapy.
Universal testing with the TST or IGRA among populations at low risk of tuberculosis generally is not recommended because either test may result in a large number of false-positive results.
A risk assessment for tuberculosis should be conducted when a new patient is first examined and on an annual basis.
Having a household member who converts (result changes from negative to positive with serial testing) on a TST or IGRA is an indication for testing a child.
Dr. Meissner is a professor of pediatrics at Floating Hospital for Children, Tufts Medical Center.
Our Trust Standards: Medical Advisory Committee